Jake Salmon recently celebrated two significant milestones -turning 21 and marking one year since finishing treatment for B cell acute lymphoblastic leukaemia (B cell ALL).
Now in remission and in his third year at Aberystwyth University studying International Politics, Jake is sharing his story to mark Teenage and Young Adult Cancer Awareness Month and in support of new research into the cancer he says put his life on hold.
Fighting fit and enjoying football and running -the active lifestyle he said he missed during treatment - he hopes future research will help transform care for young people diagnosed with leukaemia.
Jake, from Bedford, was just 17, and studying for his A-levels, when he was diagnosed with B cell ALL, an aggressive type of blood cancer that starts in young B cells. Made in the bone marrow, they normally help the body fight infections.
Jake’s body began producing too many immature cells, which crowded his bone marrow and stopped it from producing healthy blood cells. This can cause tiredness, infections and bleeding problems, and the cancerous cells can also spread to other parts of the body.

Jake said: “My symptoms were things like feeling extremely tired and fatigued, bruising very easily, having no appetite and losing quite a bit of weight. I went to my doctor, and she immediately sent me to A&E because she was worried about my breathing. I was then diagnosed in A&E after a simple blood test.”
Cancer turned Jake’s world upside down, and now he’s determined to raise awareness of the impact of facing a life‑changing diagnosis at such a formative point in young people’s lives.
“When they called me in with my parents and broke the news I had cancer, I was completely shocked,” he added. “We thought it might just have been an iron deficiency, and I didn’t really take in what the doctor was telling me until my dad took me to one side and explained what was happening. It was such a hammer blow. I went from studying to get into university and getting ready to begin my adult life, like my peers, to spending the first month of my diagnosis in hospital away from my friends undergoing multiple blood transfusions.”
Jake, who was treated at Addenbrooke’s Hospital, is grateful for the care he received. Now the clinical team who looked after him is part of a Cancer Research UK–funded project led by Dr Simon Richardson in Cambridge, which has been awarded £200,327 to continue developing kinder, more effective treatments for B cell ALL, the most common childhood cancer.
More than 600 people in the UK are diagnosed with B cell ALL each year. While the disease is curable for most children, treatment involves more than two years of chemotherapy, leaving patients vulnerable to infections and experiencing side effects such as bruising, bleeding, hair loss, nausea and vomiting, as well as potential long-term damage to nerves, joints and the heart.
Outcomes tend to be much poorer for young people and adults. That’s why researchers are urgently pursuing more effective and less toxic treatments.
Dr Richardson and his team from the Cambridge Stem Cell Institute and Department of Haematology at the University of Cambridge are trying to understand why some cases of B cell ALL are much harder to treat than others. His team looks at how young blood cells normally develop and what happens when this process goes wrong. They also study tiny chemical “switches” that help control how our genes work. When these switches stop working properly, they can help cancer grow or make it difficult to treat.

Dr Richardson, who is also an honorary consultant haematologist at Cambridge University Hospitals NHS Foundation Trust, said: “Most children with B cell ALL do well on chemotherapy, but those who relapse or who have certain genetic changes have a much lower chance of survival. B cell ALL is still one of the main causes of childhood cancer deaths, and young people and adults diagnosed with it often face even poorer outcomes.
“Many can be cured, but treatment is long, tough, and sadly still doesn’t work for everyone. A gene called CREBBP is often damaged in this cancer, especially when it comes back after treatment and this makes the leukaemia harder to treat.”
Dr Richardson’s team found that when the CREBBP gene is lost, cancer cells have to depend more heavily on other backup systems to survive. They are looking to identify these systems to find ways to block them that could kill the cancer cells, while leaving healthy cells unharmed.
He added: “Being able to shut down the ‘escape routes’ that cancer cells use to survive when the CREBBP gene is missing, would be a major breakthrough for B cell ALL patients. It could lead to more precise and less toxic treatments than traditional chemotherapy and, crucially, with fewer side effects. We’re in the early stages, but ultimately, that’s the long-term goal for this project.”
In the East of England, every year there are around 380 new cancer cases in the under 25s.
Teenagers and young adults face distinct challenges when diagnosed with the disease, from accessing appropriate medical care to managing side effects and coping with the emotional impact.
Jake said his own journey to recovery has been tough.
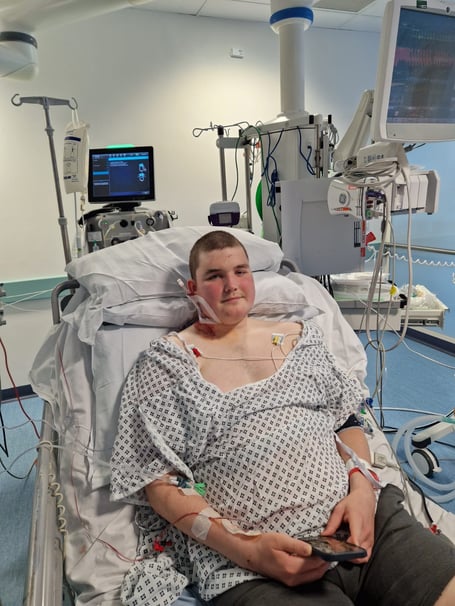
“Years of treatment affected everything from my education to my social life. The chemo was really hard and made me very ill. At one point, I was admitted to intensive care with pancreatitis caused by complications relating to my treatment. I was always worried about adverse effects and infections,” he said. “Just going to my end of year school prom was a major achievement for me and then having to tell new friends at university about my illness was a lot to deal with on top of trying to settle in and study.
“Cancer treatment isn’t easy, so my message to other young people facing a diagnosis is - don’t be too hard on yourself. I think any new research that looks at kinder treatments is a positive, and I totally support Dr Richardson and the pioneering work he’s doing to help people like me recover from this devastating disease. It’s incredible to think the people who helped me through treatment are now working on something that could make it easier for others.”
Cancers in young people are biologically different to those in children and older adults and vary in the types of cancers they get, the causes of cancer and how they respond to treatment. This means they need a specialised approach, which Cancer Research UK scientists are driving forward - including initiatives to help make it easier for teenagers and young adults to access clinical trials.
Cancer Research UK spokesperson for Cambridge, Patrick Keely, said: “Every year in the UK, around 240 young lives are lost to cancer and, those who do survive are often left with life‑long impacts from their treatment.
“That’s why initiatives like Teenage and Young Adult Cancer Awareness Month are vital to shine a light on some of the unique challenges faced by young people affected by cancer that our scientists are working to tackle.
Find out more or donate to vital research at cruk.org/tyacancers
.png?width=209&height=140&crop=209:145,smart&quality=75)



Comments
This article has no comments yet. Be the first to leave a comment.